
国际对儿童近视控制的隐形眼镜配件调查
Nathan Efron, Philip Morgan and co-authors collected data across 31 countries for at least 23,830 contact lens fits on children. Their data, collected from 2011 through to 2018, showed an increasing trend to prescribing both soft multifocal contacts and rigid lenses for the control of myopia, with the majority of multifocal contact lens fits taking place amongst children 8 to 15 years. The results were published in February 2020 in Contact Lens and Anterior Eye - click the heading above for the reference link.

图3来自Efron,Morgan等2020年 - 在31个国家 /地区,所有CL的比例中,软和刚性近视控制的趋势与儿童的比例相适应。
The authors note that during the study, the MiSight lens by CooperVision was approved in some countries (14 out of 31) as an accepted form of myopia control, which would have influenced prescribing trends.
Overall, myopia control contact lens fitting has increased from only 0.2% of contact lens fits to children in 2011 to 6.8% of fits in 2018. That's an increase of 34 times! As shown in Figure 3 above, there has been a sharp increase from 2015 in the extent of rigid CL fits for myopia control as a proportion of all rigid lens fits to children. Austria, Germany and Hong Kong led the way, with around 25% of contact lens fits to children in these countries being for myopia control.
While frequency is increasing, these are still small numbers indicating that the primary reason children are fit with contact lenses is NOT for myopia control. In commenting on this, the authors cited the lack of on-label products, perceived practitioner opinion on effectiveness and an apparent lack of myopia awareness and myopia control benefits in general. On a brighter note, the skewed age distribution of myopia control lenses fitting in younger children (average age 13, compared to average age 15 years in non-myopia control fits - see Figure 4 below) is consistent with evidence that myopia control should be prescribed at the earliest suggestions of increasing myopia.
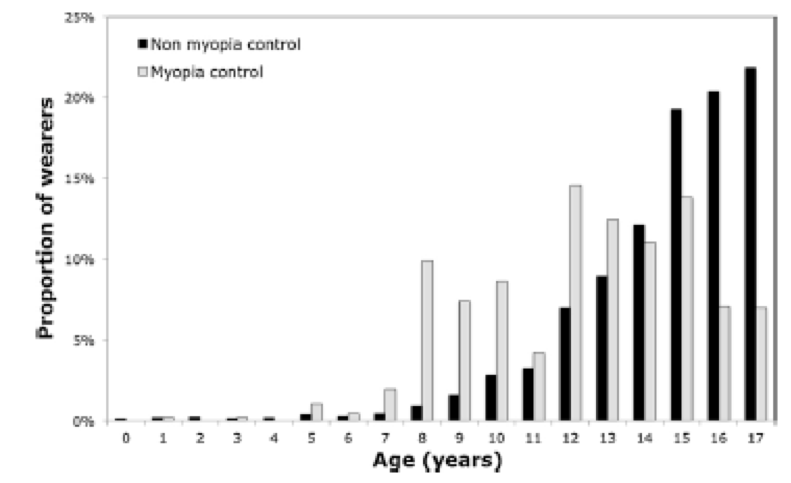
Figure 4 from Efron, Morgan et al 2020 - illustrating age categories of children fit for myopia control compared to children fit with other contact lens types.
Interestingly, no clear differences were seen in the demographics of children fitted with hard lenses for myopia control compared to soft lenses. The authors have suggested that this implies practitioners see no difference in the familiarity or complication of fitting the different lens types. One study bias that was noted is the survey was sent to practitioners with an established interest in contact lenses, which could result in different outcomes to looking at a more “general practitioner” population base.

近视管理的全球趋势临床实践的态度和策略 - 2015年和2019年的发现
First published in 2016 in Contact Lens and Anterior Eye, James Wolffsohn, Antonio Calossi, Pauline Cho, Kate Gifford and others surveyed 971 eye care practitioners in a dozen countries and six languages to examine prescribing habits and attitudes around the world when dealing with myopia in 2015. The practitioners were asked about their level of concern about increasing rates of paediatric myopia, how effective they perceived different treatments to be, how often they implement them and the minimum myopia to spur action.
Practitioners in Asia had more concerns than other countries, with a similar level across Europe, North and South America and Australasia with a median of 7/10. Orthokeratology was perceived to be the most effective, followed by outside time and then pharmaceutical interventions. Compared to other optometrists, Asian practitioners thought; single vision, bifocal and progression lenses to be the more effective.

Table 2 from Wolffsohn et al 2016 - Global Trends in Myopia Management Attitudes and Strategies in Clinical Practice; Frequency of prescribing myopia correction options
根据反应,最受欢迎的治疗ment for young progressing myopes was single vision glasses (47%), or single vision contact lenses (15.2%). Orthokeratology (14.3%) and Progressive glasses (6.5%) featured next. Asian practitioners were the most likely to prescribe single vision glasses, and Australian optometrists the least likely. Glasses were prescribed from as young as five, however contact lenses and pharmaceuticals tended to be reserved for older children, or children with a myopia of greater than -2.00D. Most practitioners will treat when progression occurs between -0.25D to -1.00D per year, with Australian optometrists intervening at the lowest levels of change. Reassuringly, 72.7% of practitioners did not consider under-correction with single vision distance lenses effective, however those in South America and India used that strategy more often than their international counterparts.
So what was holding people back? The perception that strategies were uneconomical (35.6%), insufficient information about the strategies (33.3%) and the perceived unpredictability of outcomes (28.2%). As a group researchers found that Orthokeratology was correctly agreed to be one of the most effective methods, but largely people were overestimating the impact of recommending outdoor time and underappreciating the role of pharmaceuticals. Over two thirds of children are still being prescribed single vision spectacles as the overwhelming treatment. The authors were concerned that despite growing evidence of the negative impact of myopia, and the moderate practitioner concern, update of treatments globally is poor.

Global trends in myopia management attitudes and strategies in clinical practice- 2019 Update
An update was published in 2020,[链接到开放访问纸]
This time with 1336 respondents from 16 countries, the authors highlighted in this 2020 update that "uptake of appropriate techniques has improved, but remains generally poor; this is despite growing evidence of the negative impact of even low levels of myopia on health economics and moderate levels of practitioner concern and perceived activity, particularly where the prevalence of myopia is highest."
下面的表2(从2020年的论文中)可以直接与上面的表2进行比较。在澳大利亚从业者处方单一视觉的一半中,可以看到最大的变化,药物和多焦点软处方的大幅增长,以及Orthok处方的少量减少。欧洲显示出类似的趋势,尽管单视处方的减少较小。北美的趋势从单一视力到隐形眼镜以及对大洋洲和欧洲的药物选择较慢。南美和亚洲的单一视力处方率最高,从2016年到2020年维持,并且其他选择率相当静态。尽管亚洲的从业人员报告了对童年近视频率增加的最高关注程度。以及在近视控制中(与澳大利亚同事)相等的最高水平感知的临床活动 - 请参见下面的图2。
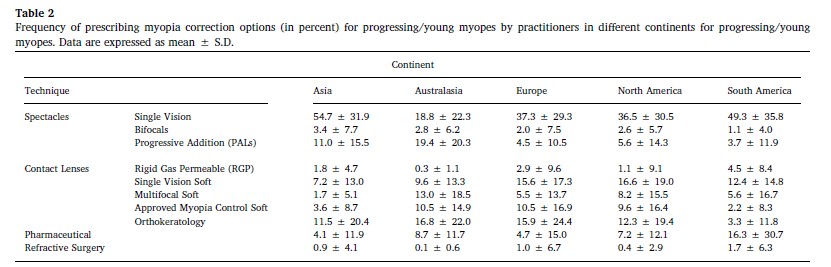
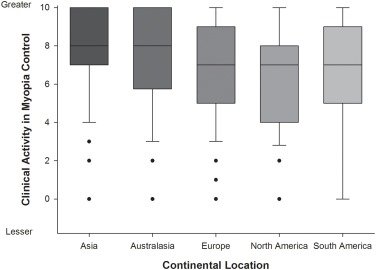
Figure 2 from Wolffsohn et al 2020 - perceived level of clinical activity in the area of myopia control for practitioners located in different continents. N = 1336. Box = 1 SD, line = median and whiskers 95 % confidence interval.
在全球范围内,大多数从业者都认为-0.75d(-0.82d +/- 0.58d)是最低的近视水平,保证纠正措施,大多数受访者感到每年的进步为-0.50d至-0.75d,需要一种形式的形式近视控制。然而,令人失望的是,全球大多数年轻的近视仍在处方单视眼镜和隐形眼镜作为最常见的校正模式,如表2所示。
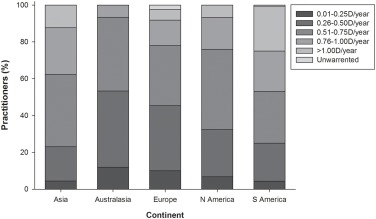
Wolffsohn等人2020年的图3-每年(D/年),每年的患者近视进展最少(DIOPTRES),该从业人员位于不同大陆的从业人员被认为需要采用近视控制方法。
更肯定的是,大多数从业人员承认,纠正不足不是近视控制的有效形式,并且自2015年以来,这个数字已经下降,但是在某些地区,尤其是在南美,它仍在实践 - 请参见下面的图4。
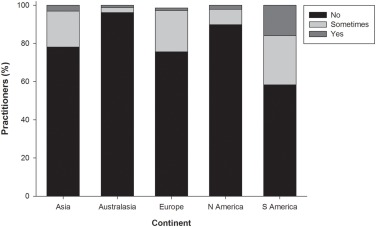
图4 2020 -使用单从Wolffsohn et al-vision distance under-correction as a strategy to slow myopia progression by practitioners located in different continents.
与2015年的论文一样,正er妇再次同意成为全球最有效的治疗方法,并反映出有关主题的教育和文献的增加,对药物控制的信心和软接触镜头的选择增加了。2019年仍然存在与2015年相同的障碍:椅子的时间增加,对治疗的有效性缺乏信心(受访者的1/3)和治疗费用(受访者的1/3)。总体而言,从业人员将开始积极的连接的近视水平已从2015年的-2.00d下降到2019年的-1.50d,但考虑到我们对儿童中近视和近视的近视预测的了解,等待主动干预的中等水平可能迟到。
As the enormous body of evidence continues to grow, education of practitioners increases and regulatory bodies catch up with new treatments available, indicators of proactive management - age at which to commence intervention and the rate of change for intervention - will continue to improve globally. However, single vision corrections are still prescribed to 52% of progressing and/or young myopes in 2019 compared to 68% in 2015. This is an improvement, but there is still a long way to go to align with best practice. In the interim, continuing to advocate, educate and discuss myopia management is crucial for clinicians and educators alike.








